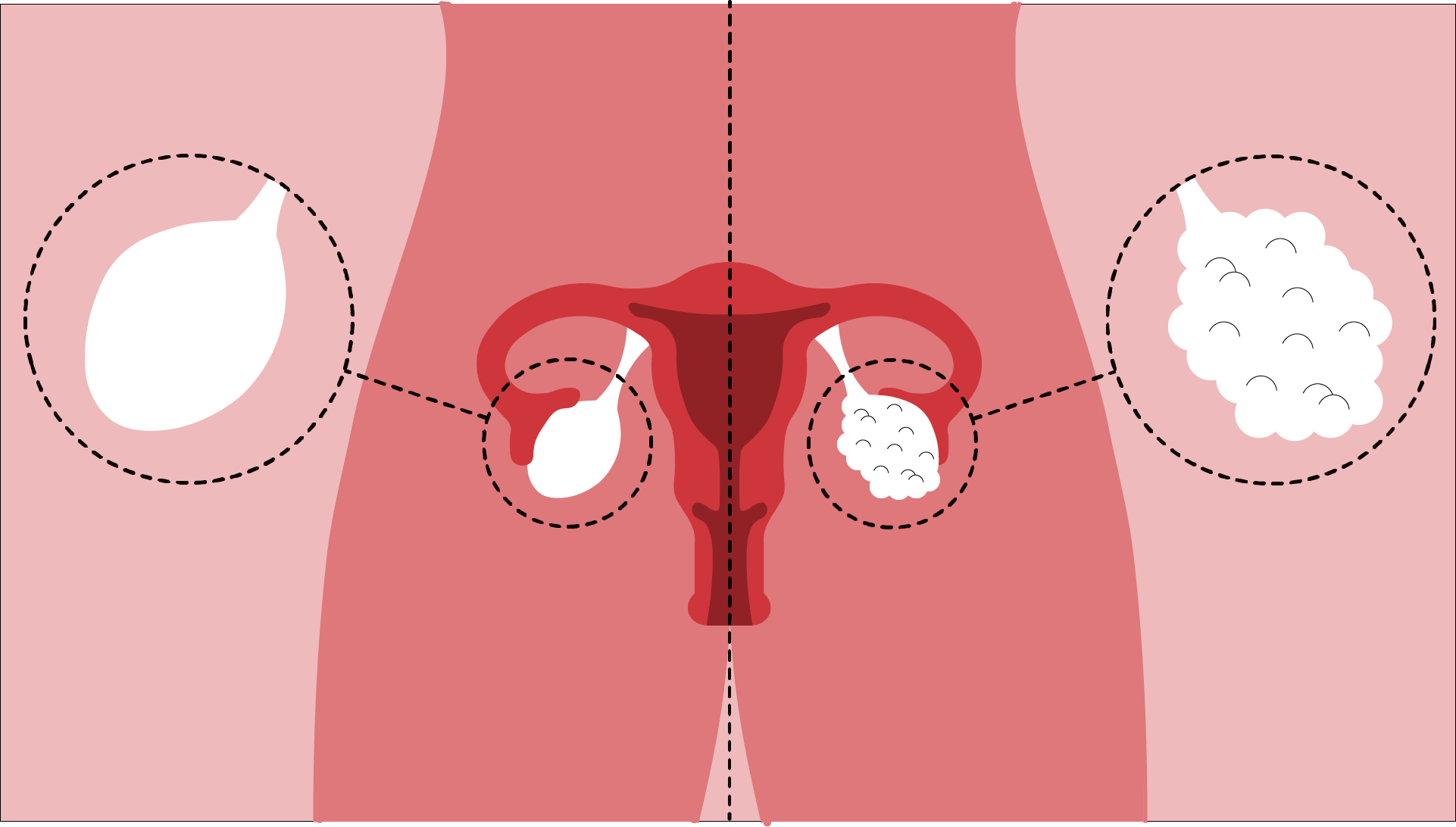
Polycystic Ovarian Syndrome, commonly referred to as PCOS, is estimated to affect five to six million women in the United States. Yet, it still remains a widely misdiagnosed and misunderstood condition.
With up to 70% of affected people with uteri remaining undiagnosed worldwide, PCOS is a common disorder that can cause hormonal imbalances, irregular periods and cysts in the ovaries.
When acne popped up, and facial hair started randomly appearing on her chin, 23-year-old Dearborn resident Zeinab Khattab had no idea what was going on, but knew something was off.
After various doctors appointments, where she was told her symptoms were "just part of growing up," Khattab did some of her own research and eventually insisted that she be tested for PCOS.
After some ultrasounds and blood tests, Khattab was officially diagnosed.
"I honestly thought it was endometriosis at first,' Khattab said, "Just based on some of the symptoms I had read online. But, upon further examination, we learned that it was PCOS. It took a couple years from first going to the doctor to finally getting a diagnosis."
Khattab said it took seeking out a female doctor, who was able to understand that her symptoms were out of the ordinary, to finally get diagnosed.
"I think one of the main issues is that a lot of these symptoms are often chalked up to just being regular 'woman issues,'" she said, "Rather than it being a serious medical concern."
Because there is no official cure for PCOS, those with the condition have to pick from a variety of treatments, such as hormone therapy or diet changes. One of the most common treatments is hormonal birth control, which Khattab didn't want to take for personal reasons.
"Ultimately," Khattab said, "I just wanted to manage the current symptoms that were concerning me, which (were) the acne and the hair growth. My doctor prescribed me Spironolactone, which is technically a blood pressure medication, but it can also be used to treat hormonal acne and excessive hair growth caused by PCOS."
Professor of pediatrics, obstetrics and gynecology and molecular and integrative physiology at University of Michigan School of Public Health Vasantha Padmanabhan is an expert on PCOS, and researches its origins through the use of animal models.
Padmanabhan said that most of the time, the first line of treatment for PCOS is oral contraceptives, such as birth control.
However, lifestyle changes — such as diet and exercise — and medications like Metformin, an insulin sensitizer, can also help women because those with PCOS are prone to diabetes or cardiovascular consequences, Padmanabhan said.
Padmanabhan added it is important for public health officials to get into "prevention mode" when addressing PCOS, because children of PCOS-affected women are also at high risk.
"There's genetic evidence saying there's a high probability of them getting some of these disorders," she said.
In her research, Padmanabhan uses sheep models to create a PCOS phenotype by exposing pregnant sheep to excess androgen levels, as well as other environmental factors linked to PCOS. She said the goal is to develop preventative treatments.
Brooke Meneima is a physical therapist and the Director of Pelvic Health at i’move, a Michigan physical therapy organization. Meneima often works with PCOS patients who suffer from related pelvic or back pain.
Because PCOS is inflammatory in nature, Meneima said, clients with the condition come in for therapy to address a variety of issues, such as muscle tension or abdominal pain. Other times, she works with patients to discuss specific diets that reduce inflammation.
Khattab said when she first began experiencing symptoms, the biggest impact PCOS had was on her confidence.
"Right after I got diagnosed," Khattab said, "We kind of went into COVID and wore masks, to the point where ... going out without a mask even a few years after I’d been diagnosed was a struggle."
Support student media!
Please consider donating to The State News and help fund the future of journalism.
Now that she has gotten older, and with her wedding approaching, Khattab said, she is mainly concerned about how PCOS may impact her fertility, as the condition is one of the most common causes of infertility in women.
Padmanabhan said more research needs to be done on PCOS.
"I don't think there's enough done," she said, "Because it's one of the major infertility disorders, and then the long term consequences in terms of comorbidities are all quite high, both psychological and metabolic in all aspects. I think there needs to be a lot more (research)."
Meinmea said the healthcare industry doesn't pay enough attention to conditions impacting those with female anatomy.
"I'm grateful conditions such as PCOS are getting to be more well known," Meinema said, "But, there is always a large gap between awareness and understanding. By normalizing conversations and asking questions, we can lead to much earlier diagnosis and reduce the future impact of conditions like PCOS."
Discussion
Share and discuss “Not 'just woman issues': Living with PCOS” on social media.